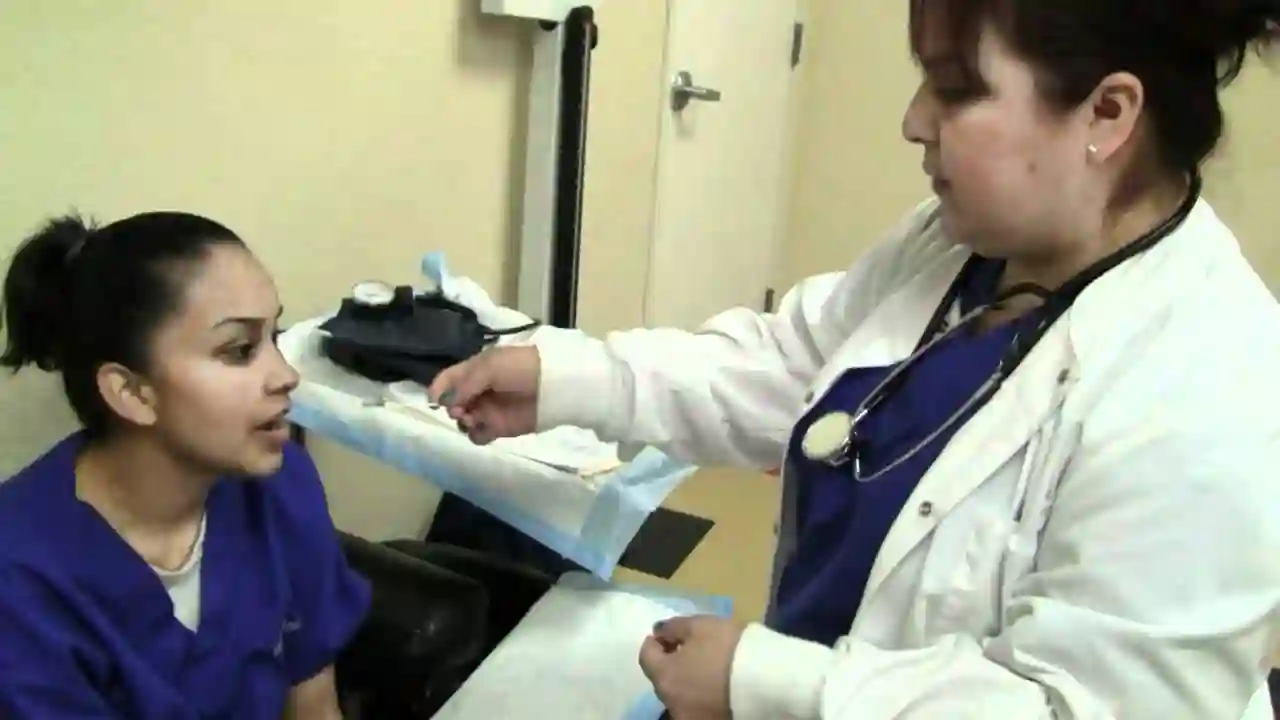
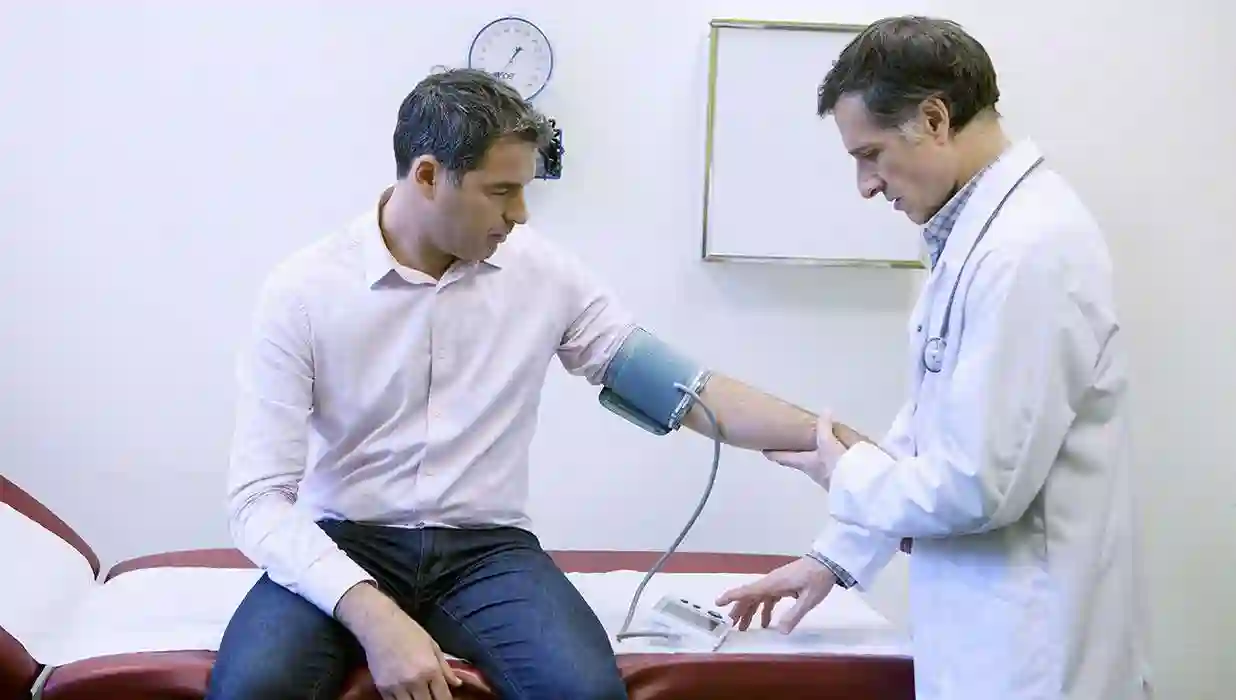
Financially, it can be extremely stressful in these unsettling times with all the shifting regulations about how claims are made, handled, and processed by insurance carriers. The most typical inquiries are… Am I obtaining the most money possible? How can I be sure I’m gathering as much as I can? How can I make more money? Maybe a medical billing service may provide all of these answers and ease the anxiety they cause. The advantages of a medical billing service are numerous. Six advantages are discussed in more detail below.
Using a medical billing service can boost collection rates
Medical billing is much more than just data entry, despite the common misconception that it is. There must be follow-up on the claims in order to collect the maximum amount of money from the submitted claims. Depending on the number of staff members in the department, claim filing and payment posting take precedence, which is frequently where internal billing falls short.
For example, if a two-physician practice has one biller who sees a fair number of patients per day, the biller will spend most of their time drafting, filing, and posting payments for claims. It takes time to enter the claims and to review each claim before sending it to the insurance company. This is also true of payment posting; even if it takes time, it is crucial to post the money received to each CPT code. There isn’t much time left for the assertions that call for additional action with only those two obligations.
The majority of the time, the denied claims can be compensated with little effort. To follow up with the insurance provider and find out what is necessary to get the claim settled, though, does take time. A full-time job is required just for follow-up. Best Medical Billing School in Pasadena service employs a number of people to work for your business. There is frequently one full-time employee who is responsible for investigating all claims that call for further action. Most Medical Billing Services offer claim follow-up as a regular function of Claim Processing rather than paying for two full-time workers.
Benefit More from a Medical Billing Service
Staff availability, eligibility services, and CPT trends are just a few of the many ways a Medical Billing Service may boost a Medical Practice’s profitability. You get several billers working on your account when you use a medical billing service. Submission of claims, posting of payments, follow-up, patient billing, and account queries are ongoing activities.
There are several billers available to cover for any absent billers, ensuring that no work is left unfinished until the absent biller returns to the office. In other words, there is no hiccup in the revenue collected or in the billing process. One of the simplest ways to guarantee appropriate payment of claims is to check patient eligibility. The patient’s eligibility has been confirmed before they ever enter the building.
As a result, the practice is assured that the patient is currently covered by the insurance company listed on their file and that any necessary referrals have been obtained. Additionally, it enables any Insurance Carrier issues (such as a change in insurance, an incorrect ID number, etc.) to be resolved before the visit, increasing the number of “clean” claims and, thus, the practice’s profit. CPT trending is yet another technique to boost a medical billing service’s profitability.
The billers frequently notice a pattern about which CPT codes are being paid and how much is being received per code when payments are submitted to CPT codes. This frequently results in two distinct outcomes. One of them is that some codes do not receive payment, which gives the practice the option of continuing to supply that service to patients or finding an equivalent or substitute service that they can offer that will receive payment.
The second scenario is where the practice frequently performs an operation, enabling a renegotiation of the amount of compensation with the insurance carrier. The three techniques mentioned above are only a few of the many ways a medical billing service can increase practice profitability.
Using a medical billing service can boost doctors’ productivity
The most crucial components of a doctor’s job—patient care—can be concentrated on when they are certain that the financial side of their practice is in capable hands and are not concerned about whether or not claims are being made and money is being collected. If a CPT code is in dispute or a diagnosis code cannot be located, a medical billing service will be able to help in identifying that code.
In consequence, this enables the doctor to continue visiting patients and charting without missing a beat rather than sitting and attempting to decipher the code. The trend that occurs when billers analyze claims before submitting them to the insurance company is comparable to CPT trending, which boosts profitability.
When there is a discrepancy in the codes being invoiced or if they notice anything being repeated, the billers will help the doctors so they may save time when writing the chart notes. Many medical billing firms give the services of a business analyst who will collaborate with the doctor and the people working in their office and offer recommendations on how to make the most of the resources available (i.e. EMR, MAs, office flow, etc). As a result, production and efficiency will grow.
Using a medical billing service can boost employee productivity
Some medical billing services give training on how to register patients correctly, collect co-payments, and design an ideal office flow that will boost productivity across the board in addition to the skills of a business analyst. Many office workers are unaware of the significance of their work and how they affect patients’ first impressions when they enter the building.
A well trained office staff will devote more time to the patients, which will be appreciated by them and increase the likelihood that they will refer the doctor to their friends and family. A medical billing service not only makes the office more efficient but also reduces the number of patient calls about their accounts. The Medical Billing Service answers calls from patients who have questions about statements or bills they have received from the office or an insurance provider. Without the strain of needing to check patients in, answer the phone, etc., they may help your patient in a professional manner. Patients can feel confident that their queries and concerns are being addressed appropriately thanks to the Medical Billing Service staff’s attention to detail and business-like demeanor.
With the help of a medical billing service, reduce claim denials
Each claim that is submitted by a medical billing service is examined by staff members who are specifically assigned to your practice to ensure that it is a “clean” claim. A “clean” claim is exactly what it sounds like; it is a claim that includes the necessary patient and insurance information, as well as the correct CPT codes that correspond to the diagnosis codes.
This lessens the possibility of an insurance company denial. Medical Billing Services make sure that the insurance company receives the greatest number of “clean” claims feasible. The amount of labor required to follow up on claims is reduced, and the practice receives more money as a result. Medical Billing Services are aware that the time spent examining claims to make sure they adhere to the requirements of the insurance carrier is time well spent.